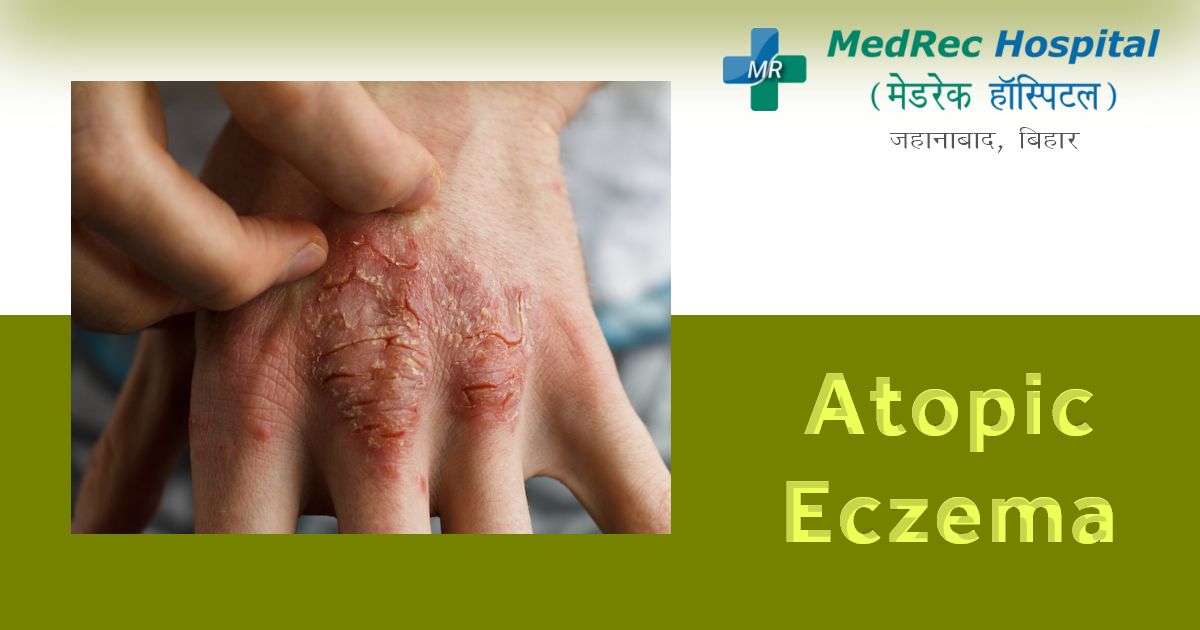
Atopic Eczema: Causes, Symptoms and Treatment Options
766
The most common type of eczema, which causes the skin to become itchy, dry, and cracked, is atopic eczema (atopic dermatitis).
Children are more likely to acquire atopic eczema, frequently before their first birthday. However, adults may also experience it for the first time at a later age.
Even though it is typically a long-term (chronic) disease, some children may have considerable improvements or even total recovery as they grow older.
Causes
Atopic eczema's specific cause is unknown, however, there are several contributing factors.
Atopic eczema frequently develops in individuals with allergies. Atopic refers to allergy sensitivity. It can run in families and frequently appears in conjunction with other illnesses like hay fever and asthma.
Atopic eczema symptoms are frequently brought on by certain triggers, including soaps, detergents, stress, and the environment. Food allergies occasionally can be a factor, especially in young children who have severe eczema.
How to check if you have Atopic Eczema?
If you have atopic eczema symptoms, visit a doctor. They can determine if you have atopic eczema by examining your skin and asking you questions like these:
- If the rash is irritating, where it initially occurs, whether it persists over time, whether there is a family history of atopic eczema, and whether you have any allergies or asthma in addition to the rash.
- If your symptoms might be caused by something in your food or lifestyle.
In order to be diagnosed with atopic eczema, you typically need to have had an itch on your skin for at least three of the preceding twelve months. A doctor will examine for the following signs:
- Red skin that is clearly inflamed in the folds of your skin, such as the insides of below your knees or at your elbows
- A history of skin irritation, combined with generally dry skin over the previous 12 months.
- A history of asthma or hay fever
Risk Factors
If you have previously had eczema; allergies, hay fever, or asthma is the greatest risk factor for developing atopic eczema. Your risk is further increased if you have relatives who suffer from these disorders.
Symptoms
The skin becomes scratchy, dry, cracked, and irritated as a result of atopic eczema.
Some people simply have a few tiny spots of dry skin, but others may have extensive skin inflammation across their entire body.
On lighter skin types, inflamed skin can turn red and on darker skin types, it can turn deeper brown, purple, or grey. On darker skin, it may also be harder to see.
Although atopic eczema can affect any part of the body, in children it most frequently affects the face, scalp, backs of the knees, insides of the elbows, and hands.
Atopic eczema sufferers typically experience periods when symptoms are less noticeable and when symptoms worsen.
The signs and symptoms of atopic dermatitis (eczema) can appear anywhere on the body and differ greatly from person to person. They may consist of:
- Cracked, dry skin
- Itchiness
- Depending on your skin tone, a rash on swollen skin will have a different hue.
- Small, raised pimples on dark-skinned individuals
- Crusting and oozing
- Extra-thick skin layers
- The skin around the eyes becomes darker
- Skin that is itchy and raw from rubbing
Prevention
Creating a simple skincare routine might help stop eczema flare-ups. The following advice might lessen eczema flare ups:
- Your skin needs moisturizing at least twice every day. Shea butter, lotions, creams, and ointments all lock in moisture. A product that functions well for you should be chosen. The best one for you should ideally be odourless, safe, and cost-effective.
- Your baby's skin may benefit from petroleum jelly used to help prevent the onset of atopic eczema.
- Take a daily shower or bath. Use warm water instead of hot water, and only take a 10-minute shower or bath.
- Make use of a soft, non-soap cleaner. Select a cleanser that is fragrance, dye, and alcohol-free. Young children may typically be cleaned up with warm water.
Treatments
The symptoms of atopic eczema can be reduced with treatment and can become better over time.
However, there is presently no treatment for severe eczema, which can make it challenging to manage both physically and emotionally. Additionally, the danger of skin infections has increased.
To manage eczema and regulate its symptoms, a variety of therapies can be used, including:
- Emollients (moisturising treatments) - used daily for dry skin topical
- Corticosteroids are examples of self-care strategies
- Minimising scratching and avoiding triggers are used to lessen inflammation, redness, and itching when flare-ups occur.
Other treatments are the following:
- Bandages or special bodysuits allow the body to heal underneath
- Treatments recommended by a dermatologist for eczema in sensitive sites that are not responding to simpler treatment
- Tacrolimus or pimecrolimus is applied topically for severe itching or itch that is not controlled by antihistamines
Complications of Atopic Eczema
Atopic dermatitis (eczema) complications might be:
Hay fever and asthma. Asthma and hay fever are frequently developed in atopic dermatitis sufferers. This may occur both before and after the onset of atopic eczema.
Food sensitivities Food allergies are frequently developed in people with atopic eczema. Hives are one of the primary signs of this illness.
Scaly, persistently irritating skin An itching patch of skin is the first sign of atopic eczema. Scratching the region only temporarily relieves the pain. As scratching stimulates the skin's nerve fibres, it actually makes the skin itch more.
Skin that is brighter or darker in spots than the surrounding tissue. Post-inflammatory hyperpigmentation or hypopigmentation are the terms used to describe this problem after the rash has healed.
Infected skin. Open sores and cracks can result from repeated scratching that tears the skin. These raise the possibility of contracting viruses and bacteria. These skin diseases have the potential to spread and endanger life.
For further information please access the following resources:
Emergency : +91 89686 77907
Front Desk : +91 98018 79584
Page last reviewed: Mar 6, 2023
Next review due: Mar 6, 2025







.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)