
Maternity
Pregnancy care, delivery planning, and postnatal coordination.
MedRec Hospital and Research Centre is a multispeciality hospital in Jehanabad, Bihar, created to bring quality treatment closer to people who should not have to travel far for timely care.
Our doctors, nurses and support teams work across emergency care, maternity, paediatrics, OPD, diagnostics and surgical services with a practical focus on comfort, clarity and affordability.

MedRec Hospital Jehanabad brings maternity care, gynaecology, NICU support, paediatrics, breastfeeding guidance, and allied services together so families can move from consultation to delivery and follow-up with clearer support.


Pregnancy care, delivery planning, and postnatal coordination.

Consultation for women's health, pregnancy concerns, and obstetric care.
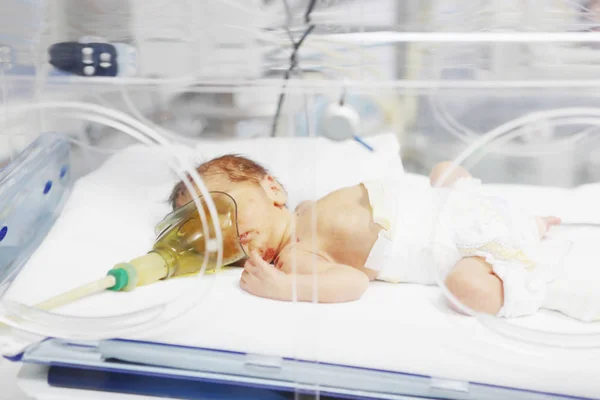
Newborn support for babies who need closer monitoring and hospital care.

Guidance for early feeding, comfort, and postnatal confidence.

Child health support from newborn needs to ongoing paediatric consultation.
MedRec Hospital is committed to simplifying the surgery journey for patients and their attendants. We offer care and assistance at every step, from pre-operative planning to post-operative recovery. Our experienced surgeons and staff are dedicated to providing the best possible care for our patients. We offer a wide range of surgical services, including minimally invasive surgery, robotic surgery, and conventional surgery. MedRec Hospital is a state-of-the-art facility that is equipped with the latest technology and equipment. We offer a comfortable and safe environment for our patients and their families.

The healthcare industry in India has inadequate emergency services due to the lack of resources. While the struggle can be noticed in cities, rural parts don’t even have the availability. This motivates us to ensure 24*7 emergency services in MedRec.
We have a team of experts to identify diseases and perform surgery for your illness related to the urinary tract system. At MedRec, we don’t just have a team of experienced doctors, we also have the state-of-the-art medical infrastructure to help them.

You can choose the medium you are most comfortable with where our experts will provide you with the best possible help available. This means, in case, you cannot make it to the hospital in time, you won’t have to compromise on the help that you can receive.

Our medical facility located at Jehanabad, Bihar is well-equipped with an OPD and a general internal medicine center. While the OPD has all the latest equipment required, the medical center further complements it by fulfilling all the required needs.

From infertility treatments to safe delivery, our experienced gynecologists and obstetricians are here to help you with women’s health-related concerns. The aim is to ensure good health for women in rural areas, just like the city.

While it’s comparatively easy for an adult to fight odds or find a treatment, children face major challenges with the same. Our dedicated team of pediatricians ensures that the children in rural areas don’t have to struggle to lead healthy life.

Stress and anxiety have become some of the most common problems in the present. While most of us ignore our mental health, at MedRec, we keep it as our topmost priority to ensure sound mental health for all.

Experience the utmost in care and precision when planning your cancer surgery with our dedicated team of medical professionals. Our personalized approach ensures that every aspect of your treatment is tailored to your unique needs and preferences. With a focus on providing comprehensive support, you can expect to be guided through every step of the process with compassion and expertise.
MedRec Hospital is committed to simplifying the surgery journey for patients and their attendants. We offer care and assistance at every step, from pre-operative planning to post-operative recovery. Our experienced surgeons and staff are dedicated to providing the best possible care for our patients. We offer a wide range of surgical services, including minimally invasive surgery, robotic surgery, and conventional surgery. MedRec Hospital is a state-of-the-art facility that is equipped with the latest technology and equipment. We offer a comfortable and safe environment for our patients and their families.
Welcome to MedRec Hospital's Cancer Center in Jehanabad, where we are dedicated to providing excellent care for those facing cancer. Our multidisciplinary team of oncologists, nurses, and support staff works as a unit to create personalized treatment plans using the latest medical technologies. We ensure each patient gets individualized attention by prioritizing comprehensive care from diagnostics to therapies.
Choose MedRec Hospital in Jehanabad for your cancer surgery, where medical expertise meets compassionate care. Our professional team is committed to helping you through a personalized and comprehensive treatment journey. We care about your well-being at every step and use good facilities and advanced surgical techniques. We also focus on holistic care beyond surgery to support your overall health and recovery. Our experienced medical team will provide the accuracy and attention your cancer surgery needs. We take a considerate approach to your specific needs and offer expert advice throughout the process.
Your healing journey starts with MedRec Hospital. Book a consultation to talk about your case, and let us plan your cancer surgery with skill, compassion, and dedication to your well-being.

Don't let medical bills stress you out. MedRec Hospital accept cashless payments from many Healthcare Insurance Providers. If yours is not on our panel, we can help you get reimbursed or claim your money back. Our team will handle the paperwork and maximize your benefits. Contact us for any questions or concerns about your bill or insurance. We're here for you and your health.

Unlock the future of female sterilization with Laparoscopic Tubal Ligation Surgery in Jehanabad !
Read Article
MedRec Hospital in Jehanabad offers advanced Knee Arthroscopy Surgery with skilled surgeons & modern
Read Article
It can be daunting to try and find the best healthcare for your children
Read Article