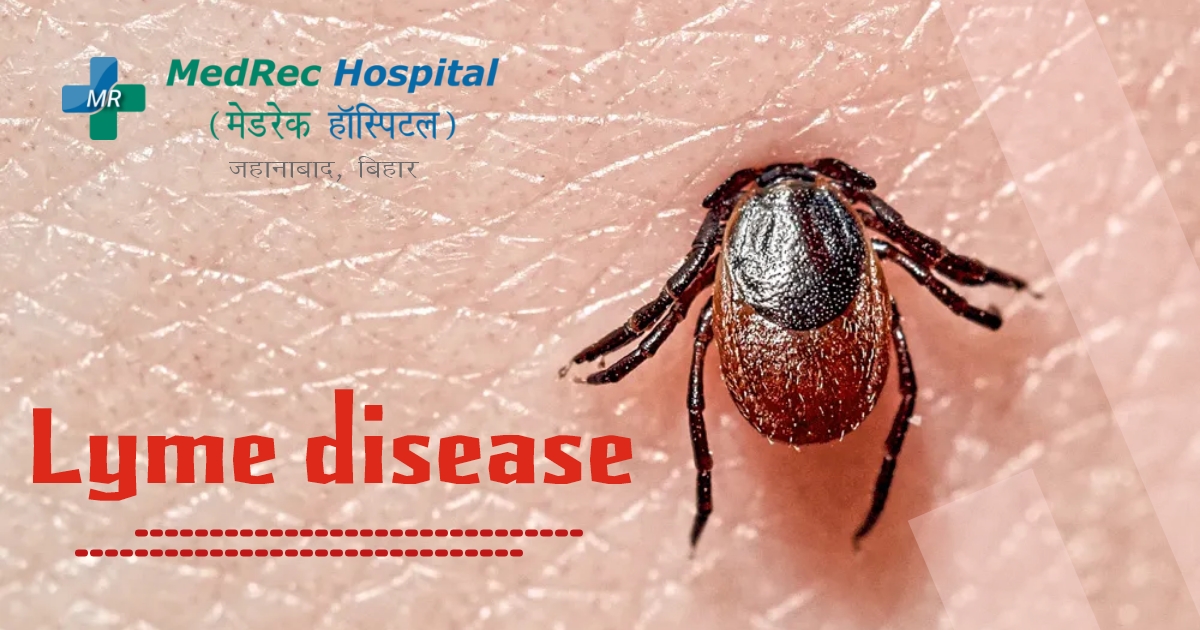
Lyme Disease Causes, Stages, Prevention And Treatment
897
Lyme disease is caused by the borrelia bacterium. A tick carrying the Lyme disease bacteria will often bite a human and spread the infection.
Ticks that can spread the bacteria borrelia can be found throughout the majority of the United States. Nonetheless, the northeastern and mid-Atlantic areas, as well as the upper Midwest, are where Lyme disease is most prevalent. Also widespread are southern and central Canada, as well as Europe.
If you spend time in regions where ticks thrive, such as grassy, brushy, or forested environments, you run the risk of contracting Lyme disease. By exercising caution, the chance of contracting Lyme disease in certain areas can be reduced.
Causes
Borrelia bacteria are the culprit behind Lyme illness. The bacteria are mostly carried by the black-legged tick, often known as the deer tick, in North America.
In Europe, Lyme disease is brought on by a different borrelia species. Bacteria are carried by ticks. These insects go by a variety of names, including castor bean ticks, sheep ticks, and deer ticks.
Biting ticks
Ticks adhere to their hosts' skin and ingest blood. The tick continues to eat until it has grown significantly in size. Deer ticks may consume blood from a host for several days.
Ticks get bacteria from their hosts, such as rodents or deer. They stay healthy. They can, however, transfer the germs to another host. The bacterium can spread when an infected tick feeds on a human. The danger of Lyme disease spreading is decreased if the tick is removed within 24 hours.
Ticks of all ages can transmit the illness. Tiny and elusive young ticks are common. If a baby tick bites you, you might not even realise it.
How to check if you have Lyme Disease?
Most patients who have Lyme disease do not recall being bitten by a tick. Moreover, many Lyme disease symptoms are also present in other diseases. If you have signs of Lyme disease, consult your doctor. Results can be improved with a prompt diagnosis and appropriate care.
Watch for signs if you know you were bitten by a tick or think you may have been exposed to ticks. Consult with your healthcare doctor as soon as you can if they appear.
Risk Factors
If you spend time in an area where they are likely to reside, your chance of contracting Lyme disease increases. This comprises the
Region. Lyme disease-carrying deer ticks are common. The upper Midwest, northeastern, and mid-Atlantic states, as well as south-central and southeast Canada, are where you may see them most frequently. There are castor bean ticks all throughout Europe.
Habitat. Ticks are found in grassy, shrubby, or forested regions.
Infection risk is highest in the spring, summer, and fall. Ticks, however, can be activated whenever it is above freezing temperature.
Symptoms
Similar to a mosquito bite, a tick bite may appear as a tiny, itchy bump on your skin. This does not imply that you have an illness spread by ticks. Many individuals will not even be aware they have been bitten by a tick.
Different Lyme disease symptoms exist. They often appear in phases. Nonetheless, the phases can mix. Also, not everyone exhibits the usual early-stage symptoms.
The earliest symptoms of Lyme disease often occur 3 to 30 days after a tick bite. There are not many symptoms present at this stage of the illness. Early localized illness is what we refer to this as.
A rash is a typical Lyme disease symptom. The rash often begins as a single circle and progressively spreads from the tick bite site. The center might grow distinct and resemble a target or bull's-eye. Although the rash frequently feels warm to the touch, it normally is not uncomfortable or unpleasant.
The following additional stage 1 signs:
- Fever
- Headache
- Extreme exhaustion
- Stiff joints
- Muscular discomfort and soreness.
- Lymph nodes with swelling.
Stage 2
Lyme illness might worsen if left untreated. During 3 to 10 weeks of a tick bite, the symptoms frequently manifest. Usually, stage 2 is more severe and extensive. The early-disseminated disease is the term for it.
Stage 2 symptoms might also include those from stage 1 and the following:
- Many rashes on various body areas.
- Neck stiffness or discomfort
- Weakness in the facial muscles on one or both sides.
- Immune system activation in the heart's tissue causes irregular heartbeats.
- Leg pain originates in the back and hips and spreads.
- Experiencing discomfort, numbness, or weakness in the hands or feet
- Edema damages the tissues of the eye or eyelid.
- Immune system activation results in discomfort or visual loss in the ocular nerves.
Stage 3
You could have additional symptoms in the third stage along with previous-stage symptoms. The late-disseminated disease is the term for this stage.
The most prevalent ailment of this stage is arthritis in big joints, especially the knees. Long-lasting discomfort, oedema, or stiffness is possible. The signs could also come and go. Stage 3 signs typically 2 to 12 months following a tick bite.
Acrodermatitis chronica atrophicans is a skin ailment that can be brought on by the kind of Lyme disease that is prevalent in Europe. The tops of the feet and the backs of the hands develop discolored, swollen skin. The knees and elbows could also be impacted. More serious circumstances might result in damage to joints or tissues.
This skin condition may manifest months or years after a tick bite.
Prevention
Avoiding tick bites when you are outside is the greatest approach to protecting yourself from Lyme disease. As you stroll or work in grassy, forested, or overgrown regions, the majority of ticks will attach themselves to your lower legs and feet. A tick will frequently move upward after attaching to your body to locate a place to burrow into your skin.
Follow these recommendations to protect yourself if you are in or intend to be in an area where ticks are likely to exist.
- Apply tick repellents.
- Spray a repellent with 0.5% permethrin on your outdoor clothes, footwear, tent, and other camping equipment. Permethrin may have been used to pre-treat certain equipment and clothes.
- On all exposed skin, excluding your own, use an insect repellent. DEET, picaridin, IR3535, oil of lemon eucalyptus (OLE), para-menthane-diol (PMD), and 2-undecanoate are a few examples of these repellents.
- Wear protective clothing.
- Wear light-coloured clothing to make it simpler for you to spot ticks on your clothing and for others to do the same.
- Do not wear sandals or shoes with exposed toes.
- Wear long sleeve shirts with your pants tucked in.
- Dress in long pants with your socks tucked in.
- Check for ticks
- To remove any loose ticks, take a shower as soon as you can. Search the area for any ticks that could have dug a hole.
- To thoroughly examine your physique, use a mirror. Take close attention to your hairline, hair, and underarms. Also, look inside your belly button, behind your knees, between your legs, your ears, and your waist.
- Check your equipment. To kill ticks, dry your outdoor clothing on high for at least 10 minutes before washing it.
Other advice
Check any pet that spends time outside every day for ticks.
In grassy and forested regions, stay as much as you can on clear routes.
Treatments
The illness Lyme is treated with antibiotics. In most cases, the faster and more complete the recovery, the earlier therapy starts.
Tablets of antibiotics
An antibiotic taken as a tablet is the typical course of therapy for Lyme disease. A typical course of therapy lasts 10 to 14 days. The length of the course of therapy will depend on your symptoms. Even if you feel better, it is still crucial to take all of your medications as prescribed.
IV medication
An antibiotic known as an intravenous (IV) antibiotic, which is administered straight into a vein, may be prescribed by your healthcare practitioner. For more severe illnesses, an IV antibiotic may be prescribed, especially if you exhibit signs of:
- Persistent arthritis
- Illness of the neurological system.
- Illness that affects the heart.
- Antibiotic usage as a preventative
An antibiotic may be recommended by your doctor as a preventative strategy.
also known as prophylaxis, but only if all three of the following occur:
- The fact that the tick that bites is a deer tick is widely recognised.
- You reside in or have recently been to a region where Lyme disease is prevalent.
- The tick was firmly fastened to the skin for at least 36 hours.
The only known therapy for Lyme disease is antibiotics. Other therapies either have not been tried or have not been proven effective.
Lyme disease-related illness
"Chronic Lyme disease" is a word that you may be familiar with. The term is often used to describe lingering symptoms that some individuals think could be connected to a previous Lyme disease sickness. However, the definition of such a phrase is vague. According to research, there is no connection between these symptoms and an ongoing borrelia-related disease.
Speak with your provider if you experience fresh health worries or persistent health issues following Lyme illness. There are several probable reasons for symptoms. Your healthcare provider can help you choose the best course of action and identify the cause of your symptoms.
Complications of Lyme Disease
Several Lyme disease patients claim that their symptoms persisted even after receiving therapy. These persistent signs might consist of:
- Lyme disease-related arthritis that does not get better.
- Body pains and discomfort.
- Fatigue that is perpetual or regular.
- Memory problems
These circumstances are not entirely understood. Some people displaying these symptoms may have PTLDS, also known as post-treatment Lyme disease syndrome. These persistent issues might be brought on by:
- Inadequate medical care.
- Getting Lyme illness again.
- Immune system reaction to dead bacterium pieces.
- Autoimmunity is the term for immune system activity that damages healthy tissues.
- Illnesses were other than Lyme disease for which a diagnosis has not been made.
For further information please access the following resources:
Emergency : +91 89686 77907
Front Desk : +91 98018 79584
Page last reviewed: Mar 17, 2023
Next review due: Mar 17, 2025







.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)