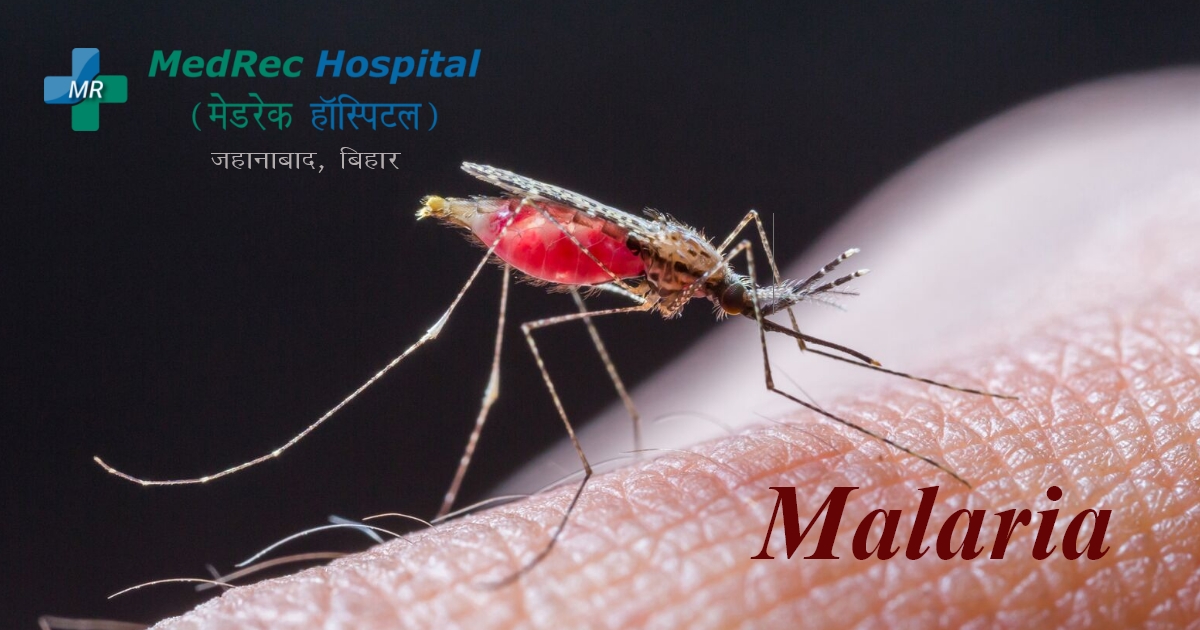
Malaria Causes, Prevention, Risk Factors & Treatment
705
A parasite can cause malaria. Mosquito bites carrying the parasite cause people to become infected. Malaria typically causes severe illness, including a high temperature and chills that cause trembling.
While malaria is rare in temperate regions, it is nevertheless common in countries that are tropical or subtropical. Malaria kills more than 400,000 people annually and affects almost 290 million people globally.
International health initiatives deliver malaria prevention medications and bed nets sprayed with insecticides to keep people safe from mosquito bites. According to the World Health Organization, children residing in nations with a high prevalence of malaria cases are advised to utilize a malaria vaccination.
While traveling, you can be protected with protective gear, bed nets, and pesticides. Moreover, you can take preventative medication prior to, during, and following a visit to a high-risk location. Common medications used to treat the disease have led to the development of widespread resistance to malaria parasites
Causes
A plasmodium-genus single-celled parasite causes malaria. Most frequently, mosquito bites are the means of parasite transmission to people. Other causes include:
The cycle of mosquito transmission
Uncontaminated mosquito. When a mosquito bites a person who has malaria, it contracts the disease.
Spread of a parasite. The next time this mosquito bites you, it might give you malaria parasites.
Within the liver. Once inside your body, the parasites go to your liver, where certain varieties can lay dormant for up to a year.
Directly into the blood. After they reach maturity, the parasites leave the liver and attack your red blood cells. People often start to exhibit signs of malaria around this time.
The next individual is now up. At this stage of the cycle, if a mosquito that is not sick bites you, it will acquire your malaria parasites and may pass them on to any more victims it nips.
Other forms of communication
People can potentially get malaria by coming into contact with contaminated blood since the parasites that cause malaria damage red blood cells, including:
- Pregnant woman to the unborn child
- By use of blood transfusions
- By exchanging drug-injecting needles
How to check if you have Malaria?
If you get a fever while residing in or shortly after leaving a place with a high risk of malaria, consult your doctor. Get immediate medical assistance if you are experiencing serious symptoms.
Risk Factors
Living in or traveling to regions where malaria is prevalent puts you at the highest risk of contracting the illness. A few of them are the tropical and subtropical areas of:
- Southern Africa
- Southeast Asia and the Pacific Islands
- North-eastern South America and Central America
The level of risk is influenced by local malaria control efforts, seasonal variations in malaria incidence, and mosquito-bite prevention measures.
Risks of more serious illness
Those who are more likely to get a severe illness include:
- Toddlers and newborns
- Older people
- Travelers from regions free of malaria
- Women who are pregnant and their unborn children
Lack of access to preventative measures, medical treatment, and knowledge exacerbates the issue in many nations with high malaria prevalence.
The capacity for immunity to diminish in malaria. Some people in a location may have been sufficiently exposed to the illness to develop partial immunity, which helps minimize the severity of malaria symptoms. If you relocate to a location where you are no longer routinely exposed to the parasite, this partial immunity may vanish.
Symptoms
Malaria symptoms and signs can include:
- Fever
- Chills
- A general uneasy sensation
- Headache
- Nausea and diarrhea
- Continent pain
- Joint or muscle aches
- Fatigue
- Quickly breathing
- Quick heartbeat
- Cough
Malaria sufferers can have recurrent "attacks." Typically, an episode begins with chills and shivering, then a high fever, followed by perspiration and a return to normal body temperature.
A few weeks after being bitten by an infected insect, malaria signs and symptoms appear. Certain malaria parasite strains, however, can slumber in your bloodstream for up to a year.
Prevention
Avoid mosquito bites if you reside in or are visiting a region where malaria is prevalent. Most mosquito activity occurs between the dark and sunrise. In order to avoid getting bitten by mosquitoes, you need to:
Shield your skin. Put on long sleeves and pants. Put your shirt in the sleeve and your pant legs in the socks.
Use skin repellent to prevent insects. On any exposed skin, use an insect repellent that has been approved by the Environmental Protection Agency. DEET, picaridin, IR3535, oil of lemon eucalyptus (OLE), para-menthane-3,8-diol (PMD), and 2-undecanoate are a few examples of these repellents. Avoid using a spray on your face. Avoid giving OLE or PMD-containing products to children under the age of 3.
Spray garments with repellant. The use of permethrin-containing sprays on garments is secure.
Go to bed with a net. The use of bed nets, especially those coated with insecticides like permethrin, can help you avoid being bitten by mosquitoes while you sleep.
Preventing illness
If you are going somewhere where malaria is frequent, consult your doctor a few months in advance to see whether you should take any medications to help protect you from malaria parasites before, during, and after your trip.
The majority of the time, the medications used to treat malaria are also used to prevent it. The medication you take will depend on where you are going, how long you will be there, and your personal health.
Vaccine
According to the World Health Organization, children residing in nations with a high prevalence of malaria cases are advised to utilise a malaria vaccination.
Researchers continue their work to research and develop malaria vaccines in order to avoid infection.
Treatments
In order to destroy the parasite, prescription medications are used to treat malaria. Drug types and duration of therapy will differ based on:
- Exactly what kind of malaria parasite do you have
- How severe are your symptoms are
The most popular antimalarial medications consist of:
Phosphate of chloroquine. Any parasites that are susceptible to chloroquine should be treated with it. Nevertheless, chloroquine is no longer a useful medication due to parasite resistance in many world regions.
Treatments are based on a combination of artemisinin (ACTs). ACT is an amalgamation of two or more medications that combat the malaria parasite in various ways. For malaria that is resistant to chloroquine, this is often the recommended therapy. Artemether-lumefantrine (Coartem) and artesunate-mefloquine are two examples.
Other typical anti-malarial medications include:
- Atovaquone-proguanil (Malarone)
- Combining doxycycline with quinine sulphate (Qualaquin) (Oracea, Vibramycin, others)
- Phosphate of primaquine
Complications of Malaria
Exceptionally when brought on by the plasmodium species that is prevalent in Africa, malaria can be lethal. According to the World Health Organization, 94% of all malaria-related fatalities are thought to take place in Africa, most frequently in children under the age of 5.
Deaths from malaria are typically caused by one or more major side effects, such as:
Brain malaria. Brain swelling or injury might result from blood cells with parasites within that obstruct tiny blood arteries to the brain (cerebral malaria). Seizures and comas might result from cerebral malaria.
Breathing issues. Breathing might be challenging if you have pulmonary oedema, which is a buildup of fluid in your lungs.
Organ malfunction. Malaria can damage or even rupture the liver, kidneys, or spleen. These illnesses all have the potential to be lethal.
Anemia. Malaria might lead to not having enough red blood cells to ensure your body's tissues receive an appropriate amount of oxygen (anemia).
Low sugar levels. Quinine, a common malaria treatment drug, as well as severe forms of the disease, can both result in low blood sugar (hypoglycemia). A coma or death may arise from extremely low blood sugar.
Certain malaria parasite strains, which normally cause less severe sickness, might linger for years and lead to relapses.
For further information please access the following resources:
Emergency : +91 89686 77907
Front Desk : +91 98018 79584
Page last reviewed: Mar 22, 2023
Next review due: Mar 22, 2025







.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)