Mastocytosis Causes, Symptoms, Prevention & Treatment
823
An uncommon condition called systemic mastocytosis causes an overabundance of mast cells to accumulate in the body. White blood cells include mast cells. All across your body, connective tissues contain mast cells. Your immune system works more effectively and naturally when mast cells are present, which helps to keep you healthy.
Excess mast cells accumulate in your skin, bone marrow, digestive tract, or other body organs when you have systemic mastocytosis. When activated, these mast cells release chemicals that can produce symptoms and indications of an allergic reaction as well as occasionally severe inflammation that may lead to organ damage. Alcohol, hot meals, bee stings, and several drugs are typical triggers.
The following are the top five forms of systemic mastocytosis:
Systemic mastocytosis is mild. This is the most prevalent kind and often excludes organ failure. Although other organs may also be damaged and the disease may steadily deteriorate over time, skin signs are frequently present.
Systemic mastocytosis that is smouldering. This kind is linked to more severe symptoms, which may include organ malfunction and a progressive illness.
Systemic mastocytosis in the presence of another bone marrow or blood disease. This severe form manifests itself quite quickly and is frequently accompanied by organ malfunction and damage.
Systemic mastocytosis that is aggressive. This uncommon form is more severe, has noticeable symptoms, and is frequently accompanied by organ malfunction and damage that worsens over time.
Mast cell cancer. This is a very uncommon and severe case of systemic mastocytosis. Most frequently, systemic mastocytosis manifests in grownups.
Skin-only, cutaneous mastocytosis is another kind of mastocytosis that mainly affects youngsters. Usually, it does not develop into systemic mastocytosis.
Causes
A random alteration (mutation) in the KIT gene is what causes the majority of instances of systemic mastocytosis. Usually, this KIT gene defect is not inherited. Mast cells are created in excess and accumulate in bodily tissues and organs, where they release chemicals like histamine, leukotrienes, and cytokines that lead to inflammation and discomfort.
How to check if you have Mastocytosis?
If you experience flushing or hives, or if any of the above-mentioned signs or symptoms worry you, consult your doctor.
Symptoms
The body component that has an overabundance of mast cells determines the signs and symptoms of systemic mastocytosis. In the skin, liver, spleen, bone marrow, or intestines, an excessive number of mast cells can accumulate. Less frequently, other organs including the heart, brain, or lungs may also be impacted.
Systemic mastocytosis symptoms and signs may include:
- Hives, flushing, or itching
- Diarrhea, vomiting, nausea, or stomach discomfort
- A bleeding disorder or anemia
- Muscle and bone discomfort
- Enlarged lymph nodes, spleen, or liver
- Depression, mood swings, or difficulty focusing
The mast cells are stimulated to release chemicals that result in inflammation and physical discomfort. Although each person's triggers are unique, the most typical ones are as follows:
- Alcohol
- Skin sensitivity
- Hot foods
- Workout
- Stinging insects
- Certain medicines
Depending on the kind, mastocytosis symptoms might change.
Dermatologic mastocytosis
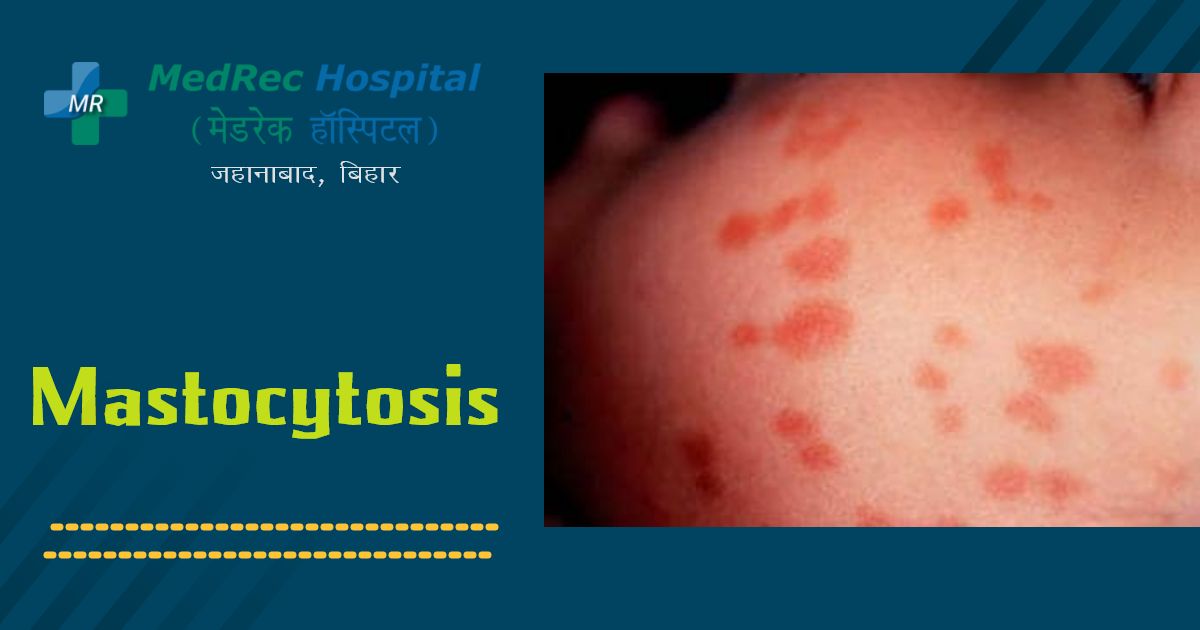
The most typical sign of cutaneous mastocytosis is the development of abnormal skin growths (lesions), such as lumps and patches that can occur on the body and occasionally blister.
Overall mastocytosis
When certain triggers, such as stress or physical activity, are present, some persons with systemic mastocytosis may have periods of severe symptoms. Many people do not have any issues.
In an episode, you could experience:
- Stomach symptoms, such as diarrhea and vomiting
- Muscular and joint discomfort, and skin responses, such as flushing and itching
- Headaches, lethargy, and changes in mood (fatigue)
Systemic mastocytosis has three primary subtypes. As follows:
- Mild to moderate symptoms of indolent systemic mastocytosis, which vary from person to person; Around 90% of cases of adult systemic mastocytosis are indolent.
- Aggressive mastocytosis occurs when mast cells multiply in organs like the spleen, liver, and digestive system; the symptoms are more severe and pervasive, though skin lesions are less frequent.
- Systemic mastocytosis with associated blood (hematological) disease occurs when a condition that affects the blood cells, like chronic leukemia, also manifests; and systemic mastocytosis without associated
Significant allergic response
Mastocytosis patients are more likely to experience a severe and perhaps fatal allergic response. Anaphylaxis is what is happening here.
The excessively high number of mast cells and their capacity to release significant quantities of histamine into the circulation contribute to the increased risk of anaphylaxis.
You may need to carry an emergency kit if you or your child has mastocytosis.
An auto-injector that delivers adrenaline can be used to treat anaphylactic symptoms.
Treatments
Depending on the kind of systemic mastocytosis and the organs affected, the course of treatment may differ. Symptom management, illness management, and ongoing monitoring are typically part of a treatment plan.
Regulating triggers
Systemic mastocytosis symptoms can be managed by recognising and avoiding anything that can activate your mast cells, such as specific foods, drugs, or insect stings.
Medications
Your doctor could suggest drugs for:
- Use antihistamines, for instance, to treat the symptoms.
- Decrease stomach acid production and intestinal pain
- Use corticosteroids, for instance, to offset the effects of the compounds generated by your mast cells.
- Limit the KIT gene's activity to lessen the generation of mast cells.
- If you have a severe allergic reaction, a medical practitioner can educate you on how to administer an epinephrine injection by yourself.
- When your mast cells are stimulated, an allergic reaction occurs.
Chemotherapy
Chemotherapy drugs may be used to treat aggressive systemic mastocytosis, systemic mastocytosis linked to another blood condition, or mast cell leukaemia in order to lower the number of mast cells.
Transfer of stem cells
A stem cell transplant could be a possibility for persons with mast cell leukaemia, an advanced type of systemic mastocytosis.
Regular observation
Using blood and urine samples, your doctor periodically assesses the state of your condition. If you are still having symptoms, you may be able to use a specialized home kit to collect blood and urine samples, which can help your doctor understand how systemic mastocytosis is affecting your body. Frequent bone density tests can keep an eye out for issues such as osteoporosis.
Mastocytosis cannot be cured, hence the goal of treatment is to lessen the symptoms.
The kind of mastocytosis and the severity of the symptoms will determine the best course of treatment.
Topical corticosteroids can be used as a short-term treatment for mild to severe instances of cutaneous mastocytosis. The amount of mast cells that may release histamine and cause swelling (inflammation) of the skin is decreased with steroid cream.
Antihistamines can also be used to treat the red skin and itching that are signs of cutaneous or indolent mastocytosis. Antihistamines are a class of drugs used to treat allergic diseases because they suppress the effects of histamine.
Complications of Mastocytosis
Systemic mastocytosis complications might include:
An allergic response. Signs and symptoms of this acute allergic response include shock, a fast heartbeat, fainting, and loss of consciousness. You could require an epinephrine injection if you experience a severe allergic response.
A disease of the blood. This may consist of anaemia and issues with blood clotting.
Stomach ulcer illness. Ulcers and internal bleeding can result from ongoing stomach discomfort.
Bones with less density. You may be at risk of developing bone conditions like osteoporosis because systemic mastocytosis can impact your bones and bone marrow.
Organ malfunction. Mast cell accumulation in bodily organs can result in organ inflammation and damage.
For further information please access the following resources:
Emergency : +91 89686 77907
Front Desk : +91 98018 79584
Page last reviewed: Mar 22, 2023
Next review due: Mar 22, 2025





.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)